Laminin Levels as a Biomarker for Liver injury in Methamphetamine Addict
DOI:
https://doi.org/10.32007/jfacmedbaghdad2477Keywords:
Laminin; , Liver function; , Liver injury; , Methamphetamine; , Toxicity.Abstract
Background: Methamphetamine (METH) is a potent synthetic stimulant that significantly impacts the central nervous system and can lead to severe liver damage. Prolonged METH use causes hepatocytes damage and fibrosis, marked by increased laminin deposition, a key component of the extracellular matrix produced by stellate cells during liver injury.
Objectives: This study aimed to investigate the effects of METH abuse on liver function and laminin (LN) levels, correlating these with the duration and concentration of METH use.
Methods: Conducted from January to August 2024, this case-control study involved 75 male participants with METH addiction (6-120 months of use) and 75 healthy controls aged 18-51. Key biomarkers were measured, including serum laminin, aspartate aminotransferase (AST), alanine aminotransferase (ALT), alkaline phosphatase (ALP), Gamma-Glutamyl Transferase (GGT), albumin and the serum concentration of methamphetamine levels.
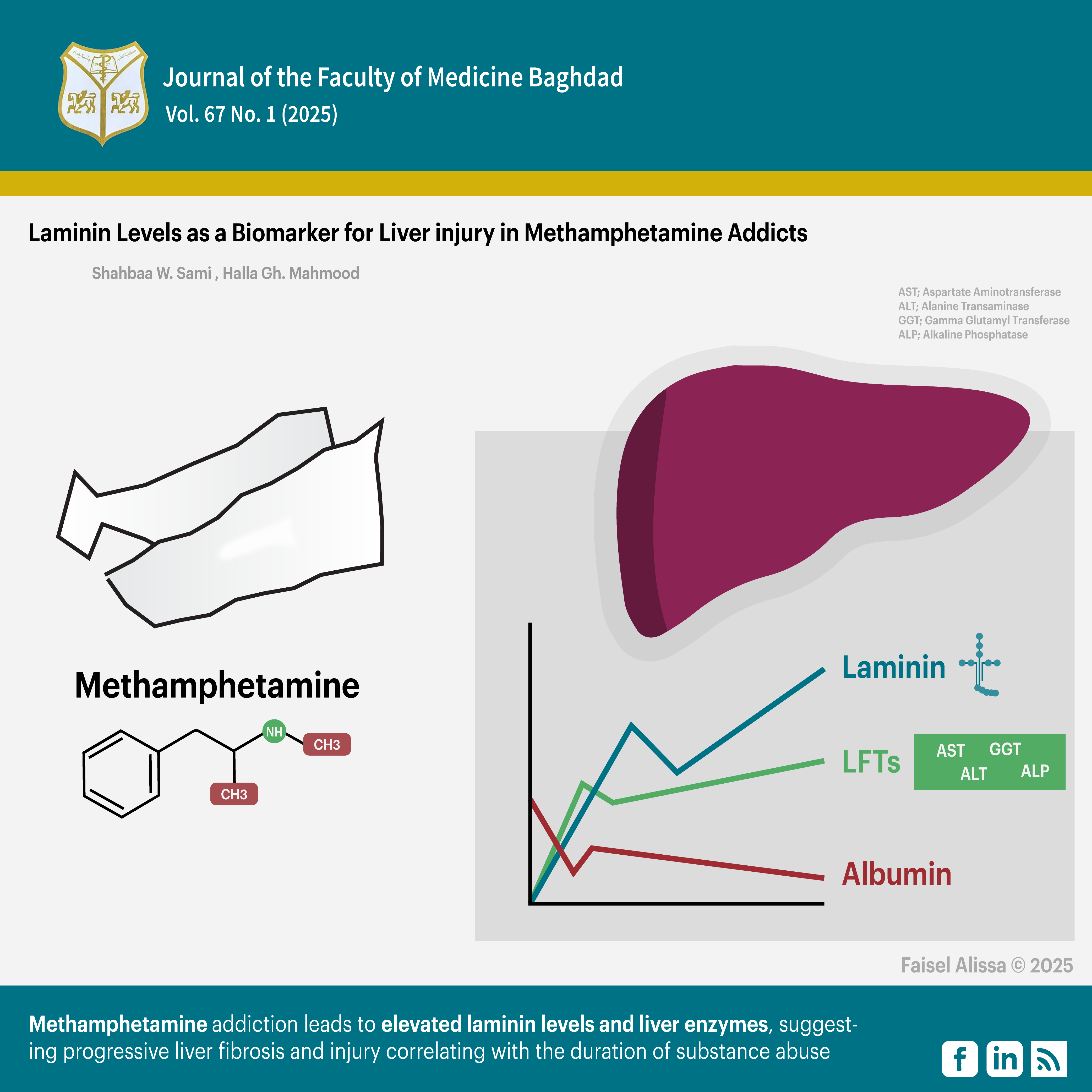
Result: The study revealed a significant increase in serum laminin, aspartate aminotransferase, alanine aminotransferase, alkaline phosphatase, and Gamma-Glutamyl Transferees. The notable significant decrease in albumin was detected. Additionally, the study demonstrated a positive correlation between LN levels and the duration of drug abuse, as between the concentration of methamphetamine levels with aspartate aminotransferase, alanine aminotransferase, alkaline phosphatase, Gamma-Glutamyl Transferees, and albumin, and correlation between methamphetamine of duration with aspartate aminotransferase, alanine aminotransferase, Gamma-Glutamyl Transferees.
Conclusions: The results indicate that METH addiction leads to elevated laminin levels and liver enzyme activity, suggesting progressive liver fibrosis and injury correlating with the duration of substance abuse.
Received: Oct. 2024
Revised: Dec. 2024
Accepted: Jan. 2025
Published April 2025
Downloads
References
1. . Gürbüzer N, Güler MC, Tör IH. Methamphetamine Use Disorder and Inflammation: A Case-Control Study. Psychiatry Investig. 2024;21(5):513-20. https://doi.org/10.30773/pi.2023.0199
2. Shahbaa Waheed Sami, Basil O. Saleh, Muataz A AL-Qazzaz. The Use of Serum Endothelin1and Myoglobin in the Evaluation of Renal Injury in Methamphetamine Abusers. Indian J Forensic Med Toxicol. 2021;15(4):3487-92.
https://doi.org/10.37506/ijfmt.v15i4.17812
3. Si Z, Yang GJ, Wang X, Yu Z, Pang Q, Zhang S, et al. An unconventional cancer-promoting function of methamphetamine in hepatocellular carcinoma. Life Sci Alliance. 2023;6(3):1-12. https://doi.org/10.26508/lsa.202201660
4. Pires B, Rosendo LM, Brinca AT, Sim AY, Barroso M, Rosado T, et al. The Therapeutic Potential of Amphetamine-like Psychostimulants. 2023;1-19. https://doi.org/10.3390/life13112180
5. Aulakh G, Singh A. A Case Report Demonstrating the Favorable Outcomes of Using N-acetylcysteine (NAC) in Managing Hepatic Injury Induced by Amphetamine-Related Drug Toxicity: Do We Underestimate Its Potential? Cureus. 2024;16(2):6-9. https://doi.org/10.7759/cureus.53697
6. Mostafa M, Nwidu E. Liver Function Abnormalities Among Substance Abusers: an in-Depth Examination. Glob J Med Pharm Sci. 2023;02(10):1-7. https://doi.org/10.55640/gjmps-abcd111
7. Asreah R, Alkagany JA. The Incidence and the Clinical Significance of the Gray Zone in the Clinical Phases of Chronic Hepatitis B Virus Infection. J Fac Med Baghdad. 2022;64(3):128-32. https://doi.org/10.32007/jfacmedbagdad.6431950
8. Addissouky TA, Ali MMA, Sayed IET El, Wang Y. Emerging advanced approaches for diagnosis and inhibition of liver fibrogenesis. Egypt J Intern Med [Internet]. 2024;36(1). Available from: https://doi.org/10.1186/s43162-024-00283-y.
9. Roy AM, Iyer R, Chakraborty S. The extracellular matrix in hepatocellular carcinoma: Mechanisms and therapeutic vulnerability. Cell Reports Med [Internet]. 2023;4(9):101170. Available from: https://doi.org/10.1016/j.xcrm.2023.101170
10. Chen Q, Mei L, Zhong R, Han P, Wen J, Han X, et al. Serum liver fibrosis markers predict hepatic decompensation in compensated cirrhosis. BMC Gastroenterol. 2023;23(1):1-11. https://doi.org/10.1186/s12876-023-02877-2
11. Elena P, Raluca Ioana A, Andrei Emilian P, Adorata Elena C. Non-invasive Serological Markers of Hepatic Fibrosis - Mini Review. Arch Surg Clin Res. 2024;8(1):032-8. https://doi.org/10.29328/journal.ascr.1001081
12. Arsana WA, Sidharta BRA, Kurniati A, Suparyatmo JB, Pramudianti MID. Diagnostic Performance of NLR, Type IV Collagen and Fibrosis Score in Chronic Hepatitis B. Indones J Clin Pathol Med Lab. 2022;28(2):149-55. https://doi.org/10.24293/ijcpml.v28i2.1826
13. Al-Imam A, Motyka MA, Hoffmann B, Al-Ka'aby H, Younus M, Al-Hemiary N, et al. Risk Factors of Suicidal Ideation in Iraqi Crystal Methamphetamine Users. Brain Sci. 2023;13(9):1-19. https://doi.org/10.3390/brainsci13091279
14. Al-Tayeb ANO, Abubakr MH, Elrheima HA, Habbani AK, Elrasul RYH. Assessment of serum creatinine, urea, and aminotransferase levels among methamphetamine addicted individuals in Khartoum State. Eur J Clin Exp Med. 2024;22(1):68-72. https://doi.org/10.15584/ejcem.2024.1.10
15. Wang L Bin, Chen LJ, Wang Q, Xie XL. Silencing the Tlr4 Gene Alleviates Methamphetamine-Induced Hepatotoxicity by Inhibiting Lipopolysaccharide-Mediated Inflammation in Mice. Int J Mol Sci. 2022;23(12). https://doi.org/10.3390/ijms23126810
16. Abdulsada HA, Taha EM. Nitric Oxide, Procalcitonin and Oxidative Stress Index Levels in Acute Bronchitis Patients. J Fac Med Baghdad. 2024;66(2):129-34. https://doi.org/10.32007/jfacmedbagdad.6622257
17. Ahmadi I, Foruozandeh H. Evaluation the multi-organs toxicity of methamphetamine (METH) in rats. Toxicol Anal Clin. 2020;32(1):4-11. https://doi.org/10.1016/j.toxac.2019.07.007
18. Alqallaf M. Toxicological Aspect of Fatal Methamphetamine. Chem Pharm Res. 2021;3(1):1-5.
https://doi.org/10.33425/2689-1050.1016
19. Sameri MJ, Belali R, Neisi N, Razliqi RN, Mard SA, Savari F, et al. Sodium Hydrosulfide Modification of Mesenchymal Stem Cell-Exosomes Improves Liver Function in CCL4-Induced Hepatic Injury in Mice. Reports Biochem Mol Biol. 2023;11(4):644-55. https://doi.org/10.52547/rbmb.11.4.644
20. Altufailia MF, Al-hakeima HK, Twaij BAA. Review on the oxidative stress in methamphetamine addicts. J Popul Ther Clin Pharmacol. 2023;30(7):421-33. https://doi.org/10.47750/jptcp.2023.30.07.046
21. Radosavljevic T, Vukicevic D, Djuretić J, Gopcevic K, Labudovic Borovic M, Stankovic S, et al. The Role of Macrophage Inhibitory Factor in TAA-Induced Liver Fibrosis in Mice: Modulatory Effects of Betaine. Biomedicines. 2024;12(6). https://doi.org/10.3390/biomedicines12061337
22. Vesterhus M, Nielsen MJ, Hov JR, Saffioti F, Manon-Jensen T, Leeming DJ, et al. Comprehensive assessment of ECM turnover using serum biomarkers establishes PBC as a high-turnover autoimmune liver disease. JHEP Reports. 2021;3(1). https://doi.org/10.1016/j.jhepr.2020.100178
23. Abbass M, Al-Hemiary N, Sahib HB. The impact of methamphetamine on psychosocial variables in patients from Iraq. Front Psychiatry [Internet]. 2024;15(September):101806. Available from: https://doi.org/10.1016/j.toxrep.2024.101806
24. Mak KM, Mei R. Basement Membrane Type IV Collagen and Laminin: An Overview of Their Biology and Value as Fibrosis Biomarkers of Liver Disease. Anat Rec. 2017;300(8):1371-90. https://doi.org/10.1002/ar.23567
25. Akhter N, Alam MA, Mian MAH, Reza HM, Islam MS. YABA (Methamphetamine tablet) administration altered cellular antioxidant status and developed fibrosis in liver of rat. Pharmacologyonline. 2019;2:269-81.
26. Anbar AP, Piran T, Farhadi M, Karimi P. Iranian crack induces hepatic injury through mitogen-activated protein kinase pathway in the liver of Wistar rat. Iran J Basic Med Sci. 2018;21(11):1179-85.
27. Verma A, Bennett J, Örme AM, Polycarpou E, Rooney B. Cocaine addicted to cytoskeletal change and a fibrosis high. Cytoskeleton. 2019;76(2):177-85. https://doi.org/10.1002/cm.21510
Downloads
Published
Issue
Section
License
Copyright (c) 2025 Halla Gh. Mahmood, Shahbaa W. Sami

This work is licensed under a Creative Commons Attribution 4.0 International License.











 Creative Commons Attribution 4.0 International license..
Creative Commons Attribution 4.0 International license..


